Liver Function Tests: What Your Results Mean and When to See a Specialist
Understanding Liver Function Tests: Key Components
If you think liver function tests (LFTs) are just another set of routine blood tests, think again. These tests are like a health report card for your liver, revealing not just how well it's functioning but also hinting at potential health issues lurking beneath the surface.
In fact, studies show that nearly 20% of people with liver disease show no symptoms until it's advanced. This is why understanding LFTs can be a game-changer in catching problems early.
The Key Players in Liver Function Tests
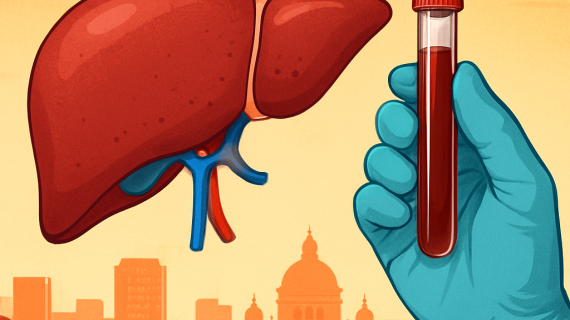
Liver function tests typically include a panel of blood tests that measure various enzymes and proteins produced by the liver. Let’s break down the key components you should know:
- Alanine aminotransferase (ALT): This enzyme is primarily found in the liver and is released into the bloodstream when liver cells are damaged.
- Aspartate aminotransferase (AST): While this enzyme is also present in the liver, it can be found in other tissues like the heart and muscles, so it’s less specific for liver damage.
- Alkaline phosphatase (ALP): Elevated levels may indicate bile duct obstruction or other liver-related issues.
- Bilirubin: This substance is produced from the breakdown of red blood cells; high levels can signal liver dysfunction or bile duct problems.
- Albumin: A protein made by the liver; low levels may suggest chronic liver disease.
Why Each Component Matters
So what? you might ask. Well, each component tells a unique story about your liver's health. For instance, if your ALT levels are elevated, it might indicate hepatitis or fatty liver disease, while high bilirubin could mean your liver isn't processing waste effectively.
Understanding these values can empower you to take charge of your health and have informed discussions with your doctor.
What Happens Next?
If any of these components come back abnormal, don't panic! Your doctor will likely recommend additional tests to pinpoint the issue. This could include imaging studies like an ultrasound or even a biopsy if necessary.
Ultimately, being proactive about your health means keeping an eye on these crucial indicators. If you're experiencing symptoms like fatigue or jaundice, it’s time to have that chat with your healthcare provider.
Common Causes of Abnormal Liver Function Test Results
Imagine receiving your liver function test results and seeing red flags waving back at you. You’re not alone; around 10% of routine blood tests reveal abnormal liver function results, and many find themselves scratching their heads, wondering what it all means.
Abnormal results can stem from a variety of issues ranging from lifestyle choices to underlying medical conditions. Understanding these causes can help you connect the dots and take proactive steps.
Lifestyle Factors
Let’s kick things off with the most common culprits: lifestyle factors. If your diet resembles a fast-food menu more than a Mediterranean feast, your liver might be crying out for help. Excessive alcohol consumption is another biggie; it’s like throwing a party for your liver but forgetting to invite the detox team.
- Obesity: Extra weight can lead to fatty liver disease, which is becoming increasingly common.
- High alcohol intake: Chronic drinking can cause inflammation and scarring of the liver.
- Sedentary lifestyle: Lack of exercise contributes to obesity and metabolic syndrome.
Medical Conditions
But I feel fine! you may say, yet some medical conditions are stealthy ninjas that sneak up on your liver without warning. Conditions like hepatitis or autoimmune diseases can wreak havoc before you even notice something's off.
- Hepatitis A, B, or C: Viral infections that inflame the liver.
- Non-alcoholic fatty liver disease (NAFLD): Fat accumulation in the liver not due to alcohol.
- Hemochromatosis: A genetic disorder causing excessive iron buildup in the body.
'Medications and Toxins
Interpreting Specific Test Results: Clinical Implications
When it comes to liver function tests, interpreting the results can feel like deciphering hieroglyphics without a Rosetta Stone. A single abnormal result can trigger a cascade of questions, and understanding what those numbers mean is crucial for your health.
Did you know that nearly 50% of patients with liver disease remain undiagnosed until they reach advanced stages? This highlights the importance of understanding your liver function results.
Let’s take a closer look at what specific test results could imply. Imagine this scenario: you recently had your liver function tests done, and your ALT levels came back elevated. While this could indicate something as benign as fatty liver disease from too many late-night pizza parties, it could also be a sign of hepatitis or even early cirrhosis.
Understanding Elevated ALT Levels
ALT (alanine aminotransferase) is like the drama queen of liver enzymes; when it’s elevated, it loves to grab attention. This enzyme is primarily found in the liver, so when it's elevated, it's often a direct signal that something's amiss. A common cause? Non-alcoholic fatty liver disease (NAFLD), which has become increasingly prevalent in urban settings like Dhaka due to lifestyle changes. If left unchecked, NAFLD can progress to more serious conditions.
What About Elevated AST Levels?
AST (aspartate aminotransferase) is the less picky sibling of ALT; it's found in various tissues including the heart and muscles. When AST levels are high, it doesn’t necessarily scream liver problem. Instead, it could be hinting at heart issues or muscle damage. But if both AST and ALT are elevated simultaneously? That’s when you should really sit up and take notice.
The Role of Bilirubin
Bilirubin is another critical player in this saga. Elevated bilirubin levels can lead to jaundice—a yellowing of the skin and eyes that’s hard to miss. It often indicates that your liver isn’t processing waste effectively or there might be an obstruction in the bile ducts. Think of bilirubin as your body’s way of waving a red flag; ignoring it could lead to more severe complications.
Ultimately, interpreting these values isn't just about numbers; it's about understanding what they mean for your overall health strategy. If you're ever unsure about your results or what steps to take next, don’t hesitate to reach out for professional guidance—especially here in Dhaka where specialized care is readily available at institutions like Popular Medical College Hospital.
When to Seek Expert Evaluation for Liver Concerns
If your liver function tests (LFTs) come back with some eyebrow-raising results, it’s not the time to play doctor with Google. In fact, nearly 20% of individuals with liver disease are completely asymptomatic until the condition becomes severe. This silent progression can make you feel like you’re in a game of medical hide-and-seek, and trust me, you don’t want to be the last one found.
Imagine this: you’re a 45-year-old professional living in Dhanmondi, juggling work and family while ignoring that persistent fatigue. You chalk it up to stress until your LFTs reveal elevated ALT and bilirubin levels. Suddenly, that fatigue isn’t just a busy lifestyle; it’s a potential signal from your liver waving a red flag.
Recognizing Warning Signs
So when should you consider seeking expert evaluation for liver concerns? Here are some telltale signs that should send you straight to a specialist like Dr. Arefin:
- Persistent fatigue that doesn’t improve with rest.
- Unexplained weight loss or gain.
- Jaundice: yellowing of the skin or eyes.
- Dark urine or pale stools.
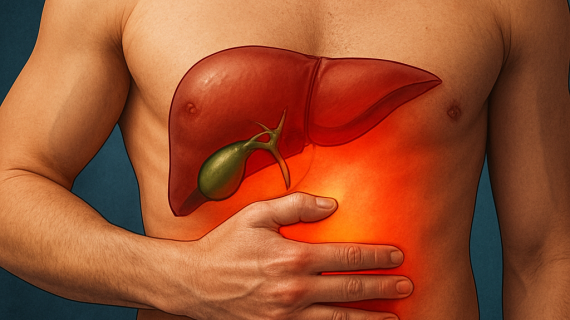
- Abdominal pain or swelling, especially in the upper right quadrant.
Note: Even if you don’t experience these symptoms but have abnormal LFT results, it's crucial to consult a specialist.
The Importance of Timely Intervention
I feel fine is a common refrain among those with liver issues. However, waiting until symptoms worsen can lead to irreversible damage. For example, if fatty liver disease progresses unchecked, it can lead to cirrhosis—a condition that drastically limits treatment options and recovery potential.
But I’m healthy!—you might argue. Yet conditions like non-alcoholic fatty liver disease (NAFLD) can develop silently over years without any noticeable symptoms until significant damage has occurred. This is why having regular check-ups and understanding your LFT results is vital for maintaining optimal health.
What Happens When You Consult an Expert?
Consulting an expert like Dr. Arefin means getting personalized guidance tailored to your unique situation. Expect thorough evaluations including possible imaging studies or even biopsies if warranted—because when it comes to your liver health, no stone should be left unturned.
In Dhaka’s bustling healthcare landscape, specialized care is at your fingertips. Don’t let fear hold you back; addressing these concerns early on can lead to better outcomes and peace of mind.
Advanced Diagnostic Procedures Beyond Standard Tests
When standard liver function tests (LFTs) raise eyebrows, it’s time to think beyond the basics. In fact, advanced diagnostic procedures are often the detectives of the medical world, uncovering hidden issues that routine tests might miss. For instance, did you know that up to 30% of liver conditions can go undetected without further investigation?
Imagine a scenario where your routine LFTs show elevated ALT levels. Instead of just shrugging it off, your healthcare provider might recommend more advanced diagnostic procedures. These could include imaging techniques like MRI or CT scans and even liver biopsies to get a clearer picture of what’s happening beneath the surface.
Imaging Techniques: Seeing is Believing
Imaging studies are like high-tech windows into your liver’s world. A CT scan can reveal structural abnormalities, while an MRI provides detailed images without radiation exposure. These techniques are particularly useful for identifying tumors or assessing the extent of fibrosis in chronic liver diseases.
Key Insight: Imaging can detect conditions like hepatocellular carcinoma (liver cancer) at an earlier stage, significantly improving treatment outcomes.
The Role of Liver Biopsy
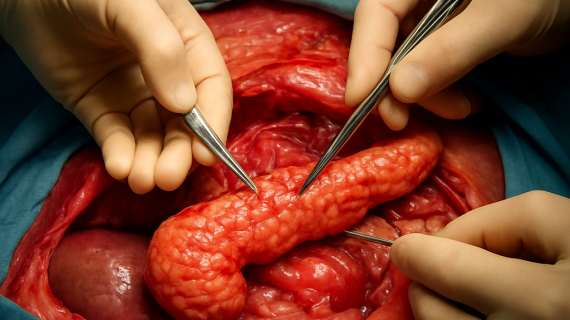
If imaging results are inconclusive or if there’s a strong suspicion of severe liver disease, a liver biopsy may be on the table. This procedure involves taking a small sample of liver tissue to analyze for inflammation, scarring, or cancer cells. While it sounds intimidating, advancements have made this procedure minimally invasive and relatively safe.
Consider this: A patient in Dhanmondi with unexplained elevated bilirubin levels underwent a biopsy that revealed early-stage cirrhosis caused by non-alcoholic fatty liver disease (NAFLD). Early intervention allowed for lifestyle changes and monitoring that significantly improved their prognosis.
Non-Invasive Alternatives: FibroScan and More
Non-invasive doesn’t mean less effective! Tools like FibroScan measure liver stiffness to assess fibrosis without any needles involved. This is particularly beneficial for patients who want to avoid invasive procedures while still getting accurate evaluations of their liver health.
In fact, studies show that FibroScan can provide results comparable to traditional biopsies in assessing fibrosis severity while being more comfortable for patients.
Ultimately, understanding the full scope of your liver health is vital. If you’re facing abnormal test results or persistent symptoms, consider discussing these advanced diagnostic options with Dr. Arefin at Popular Medical College Hospital in Dhaka. The right diagnosis could lead you down a path toward better health.
Integrating Lifestyle Modifications with Liver Health Management
Your liver is the unsung hero of your body, tirelessly detoxifying and processing everything from your morning coffee to that late-night pizza. But when it’s not functioning optimally, it can feel like you’re driving a car with a flat tire — you might still be moving, but it’s a bumpy ride. Integrating lifestyle modifications can be the key to ensuring your liver gets back on track.
A staggering 25% of adults in urban areas like Dhaka are estimated to have non-alcoholic fatty liver disease (NAFLD), often linked to poor dietary choices and sedentary lifestyles. This means that if you’re living in Dhanmondi and indulging in too many fried snacks while binge-watching your favorite series, you might just be part of that statistic.
The Power of Nutrition
First off, let’s talk about food. Think of your liver as a delicate garden; it flourishes with the right nutrients but can quickly become overrun with weeds if fed junk. Incorporating more fruits, vegetables, whole grains, and healthy fats into your diet can work wonders for liver health. Foods rich in antioxidants like berries and leafy greens help combat oxidative stress, while omega-3 fatty acids found in fish can reduce liver fat.
- Increase fruits and vegetables: Aim for a colorful plate.
- Choose whole grains over refined carbs: Say goodbye to white bread.
- Limit saturated fats: Swap out butter for olive oil.
- Stay hydrated: Water is your best friend!
The Role of Exercise
But I don’t have time! — a common refrain when exercise is mentioned. Yet regular physical activity doesn’t mean hitting the gym for hours on end; even brisk walking or dancing around your living room counts! Aim for at least 150 minutes of moderate-intensity exercise per week. This helps reduce liver fat and improves overall metabolic health.
Just 30 minutes a day can make a difference!
Say No to Alcohol
Moderation is the keyword here. Excessive alcohol consumption puts immense strain on your liver, leading to inflammation and potential long-term damage. If you’re used to unwinding with drinks after work, consider swapping them out for healthier alternatives like herbal teas or sparkling water infused with lemon.
Patient Case Studies: Real-World Applications of Liver Function Test Interpretations
Consider the case of a 50-year-old businessman from Dhanmondi who walked into Dr. Arefin's clinic, looking perfectly fine but feeling unusually fatigued. He brushed off his fatigue as a byproduct of his busy lifestyle, but his liver function tests told a different story. His ALT and AST levels were elevated, hinting at potential liver issues that could escalate if left unchecked.
This scenario is more common than you might think; about 10% of routine blood tests reveal abnormal liver function results, often without any visible symptoms. This is where understanding the implications of these tests can truly make a difference.
Case Study: The Silent Struggler
Let’s dive deeper into our businessman’s case. After reviewing his elevated liver enzymes, Dr. Arefin recommended additional imaging studies to investigate further. An ultrasound revealed fatty deposits in his liver—a clear indication of non-alcoholic fatty liver disease (NAFLD). Armed with this information, the doctor crafted a personalized plan that included dietary changes and a tailored exercise regimen.
Within months, our patient not only felt more energetic but also saw improvements in his test results. His story exemplifies how proactive management and understanding one’s liver function can lead to significant health improvements.
Case Study: The Unforeseen Diagnosis
Now let’s look at another case—a 60-year-old woman who visited Dr. Arefin due to unexplained weight loss and jaundice. Her LFTs showed elevated bilirubin levels alongside high ALT and AST values, which raised red flags for potential bile duct obstruction or hepatitis.
Further testing, including a biopsy, confirmed early-stage hepatitis C—a condition she was unaware she had been harboring for years. This timely diagnosis allowed her to start antiviral treatment promptly, drastically improving her prognosis.
Takeaway: These cases illustrate that what may seem like minor symptoms can lead to serious health concerns if not properly evaluated through liver function tests.