Gallbladder Health: Common Conditions and Surgical Solutions
When it comes to gallbladder health, understanding the common conditions that can affect this small but mighty organ is crucial for maintaining overall well-being. From gallstones to cholecystitis, many individuals in Dhaka may experience symptoms that lead them to seek expert surgical solutions. In this post, we’ll explore the function of the gallbladder, the signs of potential issues, and the minimally invasive treatments available at Popular Medical College Hospital to help you reclaim your digestive health with confidence.
Gallstones: Causes and Symptoms
Gallstones are hardened deposits that form in the gallbladder, a small organ located beneath the liver. These stones can vary in size and may consist of cholesterol or bilirubin. The formation of gallstones often occurs when there is an imbalance in the substances that make up bile, which is produced by the liver to aid in digestion.
Common Symptoms of Gallstones
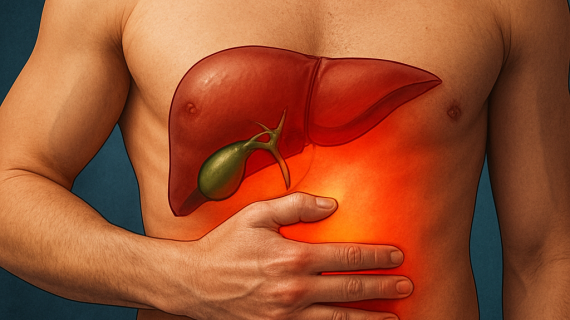
Patients frequently experience gallbladder pain, particularly in the upper right abdomen, which can radiate to the back or right shoulder. Other symptoms may include nausea, indigestion, and bloating after meals. In some cases, individuals might not notice any symptoms until a stone blocks a bile duct, leading to more severe complications.
- Sharp pain in the upper right abdomen or center of your abdomen.
- Nausea or vomiting that occurs suddenly.
- Indigestion or bloating after eating fatty meals.
Not all gallstones cause symptoms; many individuals remain asymptomatic.
A common scenario is a patient experiencing sudden abdominal pain after consuming a rich meal. This discomfort often indicates that a gallstone has moved and obstructed a bile duct. In such instances, timely medical evaluation is crucial to prevent further complications like acute cholecystitis or pancreatitis.
Many people mistakenly believe that gallstones only affect those who are overweight or have poor diets. While these factors do contribute to risk, genetics and age also play significant roles in stone formation. Understanding these nuances helps in taking preventive measures and recognizing early signs of gallbladder issues.
Cholecystitis: Inflammation of the Gallbladder
Cholecystitis is primarily characterized by inflammation of the gallbladder, often resulting from gallstones blocking the cystic duct. This blockage can lead to bile accumulation, causing irritation and inflammation. Additionally, infections can exacerbate this condition, further complicating recovery and treatment.
Causes of Cholecystitis Including Gallstones and Infection
The most common cause of cholecystitis is acute cholecystitis, usually triggered by gallstones. When a stone obstructs the cystic duct, bile cannot exit the gallbladder, leading to increased pressure and inflammation. Infection may also occur if bacteria proliferate in stagnant bile. Chronic cholecystitis can develop from repeated episodes of acute inflammation or prolonged irritation.
- Gallstones: These are hardened deposits that can block bile flow.
- Infection: Bacterial infections can lead to swelling and pus formation.
Without timely treatment, cholecystitis can lead to serious complications such as perforation or abscess formation.
Symptoms Such as Severe Abdominal Pain and Fever
Patients typically present with severe abdominal pain in the upper right quadrant, which may radiate to the back or shoulder. This pain often intensifies after eating fatty meals due to increased bile production. Other symptoms include fever, nausea, vomiting, and sometimes jaundice if there is a concurrent blockage in the bile duct.
[…] For instance, a patient may experience excruciating pain after consuming a rich meal followed by fever and vomiting. This scenario often leads them to seek emergency care where imaging tests like an ultrasound can confirm cholecystitis.
[…] A common misconception is that all patients with gallstones will develop cholecystitis; however, many individuals remain asymptomatic throughout their lives. Understanding personal risk factors—like obesity or family history—can help in early identification of potential issues.
Bile Duct Obstruction: Understanding the Condition
Bile duct obstruction poses significant challenges for gallbladder health, often stemming from various causes such as gallstones, tumors, or strictures. When bile cannot flow freely from the liver and gallbladder into the small intestine, it can lead to serious complications. This obstruction disrupts normal digestive processes and may result in elevated bilirubin levels in the blood.
Causes Including Gallstones, Tumors, or Strictures
Gallstones are a leading cause of bile duct obstruction. When a stone migrates from the gallbladder into the bile duct, it can block bile flow and lead to intense discomfort and potential infections. Tumors in or around the bile ducts may also cause obstructions by physically blocking the passage. Strictures, which are narrowings of the duct due to inflammation or previous surgery, can further complicate this condition.
- Gallstones: Hardened deposits that can block bile flow.
- Tumors: Abnormal growths that may compress or invade bile ducts.
- Strictures: Narrowing caused by inflammation or surgical scarring.
Prompt identification of the cause is crucial for effective treatment.
Symptoms Like Jaundice and Dark Urine
Symptoms of bile duct obstruction often manifest as jaundice—yellowing of the skin and eyes—alongside dark urine. These symptoms indicate an accumulation of bilirubin due to blocked bile flow. Patients may also experience severe abdominal pain, particularly if there is concurrent inflammation in the gallbladder or pancreas.
[…] For example, a patient might notice their urine becoming darker over several days while simultaneously experiencing increasing abdominal discomfort after meals. Such signs warrant immediate medical attention to prevent further complications like cholangitis (infection of the bile duct) or pancreatitis.
[…] A common misconception is that only older adults face these issues; however, younger individuals with specific risk factors such as obesity or a family history of gallstones are also at risk. Recognizing these symptoms early can significantly impact treatment outcomes.
Diagnosis of Gallbladder Conditions
Accurate diagnosis of gallbladder conditions is essential for effective treatment. Given the complexity of the biliary system, a range of diagnostic tests is employed to identify issues like gallstones, cholecystitis, or bile duct obstructions. Common methods include ultrasound and MRI, both of which provide critical insights into the gallbladder's structure and function.
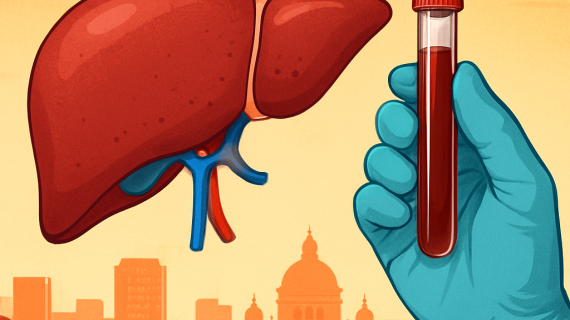
Common Diagnostic Tests Including Ultrasound and MRI
Ultrasound remains the first-line diagnostic tool due to its non-invasive nature and ability to visualize gallstones or inflammation in real-time. It is particularly effective in identifying gallstones and assessing the gallbladder's size and wall thickness. MRI may be used when further detail is necessary, especially for evaluating bile duct obstructions or complications related to tumors. While these imaging techniques are generally reliable, they are not infallible; for instance, small stones may sometimes be missed on ultrasound.
- Ultrasound: Non-invasive, quick, and effective for initial evaluation.
- MRI: Provides detailed images when more information is needed.
Early diagnosis can significantly improve treatment outcomes and prevent complications.
Importance of Accurate Diagnosis for Effective Treatment
An accurate diagnosis not only guides treatment options but also helps in anticipating potential complications. For example, if a patient presents with symptoms suggestive of acute cholecystitis but is misdiagnosed, they may face serious repercussions such as a ruptured gallbladder or severe infection. Understanding the nuances between chronic cholecystitis and other conditions can lead to different management strategies—chronic cases might benefit from lifestyle modifications alongside surgical options while acute cases may require immediate intervention.
[…] Consider a patient who initially experiences intermittent gallbladder pain that escalates after fatty meals. If diagnosed promptly with an ultrasound showing multiple small gallstones, they might be treated with dietary changes or monitored over time. However, if those stones cause an obstruction leading to jaundice or severe pain without timely intervention, the need for surgical removal could become urgent.
Laparoscopic Cholecystectomy: A Minimally Invasive Solution
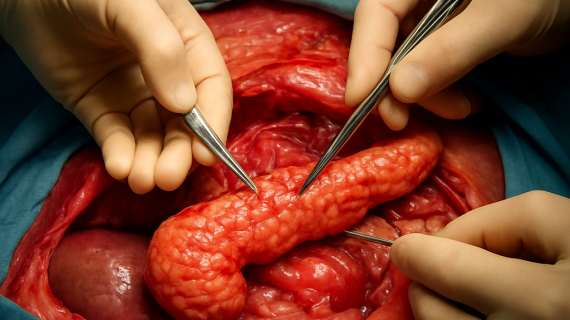
Laparoscopic cholecystectomy is the standard surgical approach for gallbladder removal, particularly when dealing with gallstones or cholecystitis. This minimally invasive procedure involves making small incisions in the abdomen through which a camera and surgical instruments are inserted. The advantages of this technique over traditional open surgery are significant, including reduced pain, shorter recovery times, and minimal scarring.
Overview of the Procedure and Its Advantages Over Traditional Surgery
During laparoscopic cholecystectomy, carbon dioxide gas is introduced into the abdominal cavity to create space for the surgeon to operate. The surgeon then uses a laparoscope, which provides a magnified view of the gallbladder on a monitor. This method allows for precise removal of the gallbladder without large incisions, facilitating quicker healing. Patients typically experience less postoperative pain and can often return to their normal activities within a week.
- Less postoperative discomfort compared to open surgery.
- Shorter hospital stay and quicker return to daily activities.
- Reduced risk of infection due to smaller incisions.
Laparoscopic surgery offers patients a faster recovery with significantly less scarring.
Typical Recovery Time and Post-Operative Care
Recovery from laparoscopic cholecystectomy is generally swift. Most patients can leave the hospital within hours after surgery, depending on their overall health and any complications that may arise. Full recovery typically occurs within one to two weeks. Post-operative care includes monitoring for signs of infection, managing pain with prescribed medications, and adhering to dietary changes as recommended by healthcare providers.
For example, a patient in Dhaka might undergo this procedure on a Thursday and be back at work by the following Monday, provided their job does not involve heavy lifting or strenuous activity. This rapid return to normalcy highlights one of the key benefits of choosing laparoscopic surgery over traditional methods.
'It's important to note that while laparoscopic procedures are generally safe, they are not without risks. Complications such as bleeding or injury to surrounding organs can occur in rare cases. Patients should have thorough discussions with their surgeons about these risks before opting for surgery.'
Open Surgery for Gallbladder Removal: When Is It Necessary?
Open surgery, known as open cholecystectomy, is sometimes necessary for gallbladder removal when complications arise that prevent the use of minimally invasive techniques. While laparoscopic surgery is preferred due to its lower risk and quicker recovery, certain conditions may warrant a more traditional approach.
Indications for Open Surgery Versus Laparoscopic Approach
Open surgery is typically indicated in cases where there are complications such as severe inflammation or scarring from previous surgeries that obstruct the surgical field. For instance, a patient suffering from chronic cholecystitis may present with dense adhesions around the gallbladder, making laparoscopic access difficult or unsafe. Additionally, if a patient has large gallstones or a suspected malignancy, an open approach allows for better visualization and management of surrounding tissues.
- Severe inflammation or infection of the gallbladder.
- Previous abdominal surgeries leading to significant scarring.
- Presence of large gallstones that could complicate laparoscopic removal.
Understanding when open surgery is necessary can help prevent complications during treatment.
Potential Risks Associated with Open Surgery
While open cholecystectomy can be lifesaving, it carries inherent risks such as increased pain, longer recovery times, and higher rates of infection compared to laparoscopic methods. The larger incision required in open surgery also increases the likelihood of postoperative complications like hernias. For example, a patient recovering from an open procedure might face several weeks of limited mobility and pain management challenges compared to those who undergo laparoscopic surgery.
Patients often underestimate the recovery time associated with open surgery, says Dr. Murshidul Arefin. While many may expect to return to normal activities within days, it can take weeks for full recuperation. This highlights the importance of thorough pre-surgical discussions with healthcare providers about potential outcomes and recovery expectations.
Post-Surgical Care: Ensuring a Smooth Recovery
Post-surgical care is crucial for patients recovering from gallbladder removal. After a cholecystectomy, whether laparoscopic or open, the body requires time to adjust to the absence of the gallbladder, which plays a role in bile storage and digestion.
Guidelines for Diet and Activity Post-Surgery
Following gallbladder surgery, patients should gradually reintroduce foods into their diet. Initially, a bland diet low in fat is recommended to minimize digestive discomfort. As recovery progresses, patients can slowly incorporate more varied foods while monitoring their body's response. It's also important to stay hydrated and avoid heavy meals that could overwhelm the digestive system.
- Start with clear liquids and progress to soft foods.
- Avoid high-fat foods for at least several weeks post-surgery.
- Limit caffeine and alcohol intake to reduce digestive strain.
Gradual dietary changes help prevent complications like diarrhea or bloating.
Signs to Watch For That May Indicate Complications
Patients should be vigilant about any unusual symptoms during recovery. Signs of complications may include persistent abdominal pain, fever, jaundice, or changes in bowel movements such as diarrhea or dark urine. These symptoms could indicate issues such as bile duct obstruction or infection.
[…] For instance, if a patient develops jaundice after surgery—a yellowing of the skin and eyes—it may suggest that bile flow has been obstructed. This requires immediate medical attention to address any underlying problems before they escalate.
[…] Many patients mistakenly believe that any post-operative discomfort is normal and may delay seeking help. Understanding what constitutes normal recovery versus signs of complications can make a significant difference in long-term health outcomes.
When to Seek Expert Care from Dr. Murshidul Arefin
Recognizing when to seek expert care for gallbladder issues is critical for effective management and treatment. Patients should consider consulting a specialist like Dr. Murshidul Arefin when experiencing persistent gallbladder pain, especially if it’s coupled with other symptoms such as jaundice, fever, or severe digestive disturbances.
Indicators that Necessitate Consultation with a Specialist
Several key indicators suggest the need for specialized care. If you experience recurrent episodes of gallbladder pain that disrupt daily activities or notice changes in your bowel movements, these could signal underlying conditions requiring surgical intervention. Additionally, symptoms like yellowing of the skin or eyes (jaundice) indicate potential bile duct obstruction and necessitate immediate evaluation.
- Persistent abdominal pain that worsens after meals.
- Nausea or vomiting that does not subside.
- Jaundice or dark urine indicating possible obstruction.
Timely consultation can prevent complications such as pancreatitis or infection.
How Dr. Arefin's Expertise Can Benefit Patients with Gallbladder Issues
Dr. Murshidul Arefin offers a wealth of experience in managing complex gallbladder conditions. His expertise allows for accurate diagnosis and tailored treatment plans that address both immediate concerns and long-term health outcomes. For instance, he employs advanced imaging techniques to evaluate the biliary system effectively, ensuring no stones are missed during diagnosis.
'In one case, a patient presented with recurrent abdominal pain and jaundice after fatty meals. Through targeted imaging and assessment, Dr. Arefin identified multiple gallstones obstructing the bile duct, leading to an urgent laparoscopic cholecystectomy. This timely intervention not only alleviated the patient's discomfort but also prevented further complications.'